Article Text
Abstract
Objective To investigate the long-term effect of medically serious adverse medical events (AMEs) among older adults.
Methods We linked nationally representative survey and claims data from the Medicare Current Beneficiary Survey (1998–2004) with non-response files (1999–2005) and the Area Resource File, providing 12 541 beneficiaries with 428 373 person-months for analysis. Latent class analysis was used to assign severity status to episodes. Multinomial logistic regression was used to identify AME risk factors. The long-term consequences of AMEs on Medicare expenditures were examined by population average models. Survival analyses examined the long-term risk of death.
Results Nearly 19% of participants experienced at least one AME, with 62% from outpatient claims. The risk of AMEs is greater among participants in poorer health, and increases with comorbidity and with impairment in performing activities of daily living or instrumental activities of daily living. Medicare expenditures during an AME episode increased sharply and remained higher than what would have otherwise been expected in quarters following an AME episode, and failed to return to pre-AME expenditure levels. Differences in survival rates were observable long after the AME episode concluded, with only 55% of the patients sustaining an AME surviving to the end of the study. In contrast, nearly 80% of those without an AME were estimated to have survived.
Conclusions The impacts of AMEs are observable over extended periods of time and are associated with considerable excess mortality and costs. Efforts to monitor and prevent AMEs in both acute care and outpatient settings are warranted.
Statistics from Altmetric.com
Introduction
The seminal report by the Institute of Medicine, ‘To Err is Human’, drew attention to the widespread problem of medical injury in the USA, indicating that 98 000 avoidable deaths occur each year as a result of adverse medical events (AMEs), which are also referred to as medical injuries.1 Although estimates vary across studies, one recent report indicated that 13.5% of hospitalised older adults experience at least one adverse event each year.2 Besides unacceptably high mortality rates, medical injuries result in longer hospital stays, increased medical costs3 and preventable disability.4 Older adults are especially vulnerable with a higher incidence of occurrence5 and poorer outcomes following AME6 in comparison with younger populations.
Improving patient safety by preventing medical injury is a key public health initiative following implementation of the Affordable Care Act. However, previous research on AME has focused on hospital settings and discrete care episodes to obtain incidence rates, and has used time frames of 6 months or less to estimate disability and mortality outcomes.7 A paucity of information exists about the occurrence of AME among older adults across the healthcare continuum as well as the long-term impact of AME on older adult outcomes.8 This dearth of information represents a critical gap in the literature base, as AMEs are likely to affect older adults in unanticipated ways. For example, Creditor9 noted that after an acute event, older adults often experience ‘a cascade of dependency’ that persists even after the original problem is treated successfully. Moreover, the risk of AMEs across medical settings is particularly important to understanding incidence and prevention of medical injury among older adults because they are frequent users of the healthcare system,10 often have complex medical needs11 and appear to have not only higher, but increasing rates of AMEs.1 In response, our objective was to conduct a longitudinal investigation of the risk of and long-term effect following medically serious AMEs among older adults using Medicare claims data from both hospital and ambulatory settings.
Methods
Data source
Three data sources were used. The core data were from the Medicare Current Beneficiary Survey (MCBS) Access to Care and Cost and Use files. The MCBS is nationally representative of all Medicare beneficiaries enrolled in the traditional (Fee-For-Service) Medicare programme. The MCBS is conducted by the Office of Strategic Planning of the Centers for Medicare and Medicaid Services, which contracts with Westat for survey and data administration. The MCBS has been continuously conducted since 1991 with participants enrolled in 4-year cohorts before rotating off. Each year, a new cohort enrols and a previous cohort completes its participation. Thus, the MCBS is a panel survey consisting of roughly 12 500 Medicare beneficiaries and combines survey data with respondent Medicare claims.12 It includes a broad set of variables which are surveyed annually, including: sociodemographics, income, living arrangements, insurance status, comorbidities and overall health, activities of daily living (ADLs), instrumental activities of daily living (IADLs), and physical functioning levels. In addition, complete Medicare claims data are available for all participants except those who are enrolled in a Medicare managed care plan. The MCBS represents the most comprehensive data source available for research investigating healthcare use, costs and outcomes among Medicare beneficiaries.13 Additional information on the MCBS is available elsewhere.14 ,15
The core MCBS files were linked with annual MCBS non-respondent files, which contain Medicare claims and administrative data, such as date of death, for non-respondents and panel retirees who survived at least 1 day of the survey calendar year, but who left the panel before completing the annual surveys as well as those who completed panel participation. This permitted the inclusion of censored beneficiaries’ service use and associated expenditures for the calendar year following respondents’ last survey interview. Data from the Area Resource File were used to control for rural–urban differences across regions. Federal Information Processing Standards (FIPS) codes were used to facilitate linkage.
Study population
Seven years (1998–2004) of MCBS survey data were linked with non-respondent claims files (1998–2005) using a unique but masked subject identifier available across all MCBS survey files and claims data. The following inclusion criteria were imposed to ensure availability of claims data for all Medicare-covered services: MCBS respondents were: (1) community-residing at the onset of panel participation, (2) aged 65 years or older on 1 January of the calendar year of their first panel survey, (3) continuously entitled to Medicare Parts A and B and (4) not enrolled in a Medicare health maintenance organisation anytime during the calendar year. Additionally, respondents sustaining an AME in the first 6 months of panel participation were omitted to avoid including potentially left-censored episodes. The final sample with complete data on all study variables consisted of 12 541 respondents who contributed 428 373 person-months of observation.
AME identification, episode construction and severity status
AMEs were identified from Medicare claims files using the Utah/Missouri Adverse Classification System of Adverse Medical Events16 for the International Classification of Diseases, Ninth Revision (ICD-9-CM) diagnostic codes: misadventures ((E870–E876)+(N998.2,.4,.7)), complications ((E878–E879)+(N996.0–996.7; 997.0–997.5; 997.9; 998.0,.1,.3,.5,.6,.8, .9)) and adverse drug events ((E930–E949 (exclude: E850.1; 854.1))+(N960–979 (exclude: 965.01))).
Episode construction began by identifying all Medicare claims with an ICD-9 code indicating a potential AME. First, claims data for respondents with at least one potential AME were identified, and then interleaved and sorted chronologically according to through-date. The first claim with an identifiable AME was identified as the index AME record. Beginning with the index AME record, episodes were defined by adding 1 month prior and 1 month post the index AME record, creating a fixed period of measurement. A 6-month clear-zone was imposed at the beginning of panel participation to guard against potential left-hand censoring.17
After potential AME episodes were identified, latent class analysis using mixture-likelihood estimation was used to determine the underlying severity of AME episodes (severity status). Latent class analysis has been used widely in cancer studies to group both patients and symptoms,18 and has been used broadly in the extant literature.19 ,20 The software package LatentGold 4.0 was used. Correlates of severity were: AME episode length, hospitalisation status, number of procedure codes, count of limitations in performing ADLs and count of limitations in performing IADLs.21 To determine AME severity, an alternative episode construction strategy which allowed episode length to vary was used to define AME length.22 In this approach, after identifying the index AME record, episodes were constructed by extending the AME window forward by each additional AME claim occurring within 180 days of the previous AME claim. If no AME claims were found, the AME episode was terminated on the end date of service of the last AME claim. These cluster solutions were then grouped into three categories representing least severe AME cases, severe AME cases and most severe AME cases. Final AME severity status was based on class membership in either of the two most severe categories. Dummy variables were specified to identify person-month observations prior to, during and after the AME episode, termed pre-AME, active-AME and post-AME, respectively, and served as the independent study variables of interest.
Dependent variables
A dummy variable indicating any AME versus otherwise was specified to permit modelling risk factors associated with experiencing an AME. A person-month level measure of total, monthly Medicare (Part A and Part B) expenditures was used for the long-term effect of AMEs on healthcare expenditures over time. Monthly total Medicare expenditures were aggregated from the following Medicare claims files: inpatient hospital stays, outpatient/ambulatory care visits, physician visits, hospice care, skilled nursing home care, home healthcare and durable medical equipment. Time until death was used to model the survival consequences following an AME.
Proxy AME
Although a medically serious AME should naturally increase short-term mortality risk due to the sequelae associated with the AME, less is known about the effect of such events over the long run. To investigate time to event outcomes, participant histories were screened to identify patient histories with and without an AME, creating two samples. For the group with an AME, the date of service on the claim file served as the index date for constructing episode windows. Using a historical cohort methodology, proxy AME dates were then randomly assigned to beneficiaries not experiencing an AME during their panel membership. Using SAS, artificial sentinel AME dates were randomly assigned to the comparison sample to allow post-AME tracking of their survival relative to a specific date within their medical service use histories. Then, using these proxy dates, episode windows were constructed for the unexposed group which permitted the comparison of histories of beneficiaries with and without an AME by tracking survival for each subgroup relative to a specific date within their medical service use histories.23 ,24 This approach was used to adjust for the bias in comparing AME occurrence and outcomes in the presence of time-dependent events with competing risks (eg, censored due to death, loss to follow-up, end-of-panel participation).25 ,26
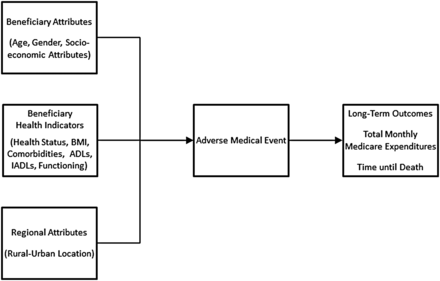
Conceptual model
For the purposes of this study, we draw upon the conceptual model advanced by Scheetz27 for exploring the relationship between beneficiary attributes (eg, age, gender, socioeconomic attributes) and beneficiary health attributes (eg, pre-existing conditions, ADLs, IADLs) on medical injury outcomes. We further modify this model to reflect the hypothesised effect of individual factors on both the risk of experiencing an AME in the short-term as illustrated by the middle box, and on the long-term risk of increased Medicare expenditures and mortality risk over the long run (see figure 1). Last, because rurally located populations tend to be both older and in poorer health than the population as a whole, which may place them at greater risk for experiencing an AME, we further modify the conceptual model to include rural–urban location.28
Conceptual model.
Independent variables
Drawing upon this framework and the broader AME literature,2 ,29–31 the following variables were considered for study inclusion and used for casemix-adjustment purposes: age, gender, marital status, race, income, education level, self-rated health, count of comorbidities, functional status, ADLs and IADLs, body weight, region of residence, and cohort membership. Except for age, race and gender, all independent variables were specified as time-varying covariates which were updated at least once with each annual beneficiary survey. Because justification for study inclusion and variable specifications are conventional, only a brief overview is provided here.
Beneficiary attributes
Beneficiary age was specified as the respondent's baseline age at the time of the first interview of panel membership. Dummy variables were specified to adjust for casemix population differences, including: male gender, income, race/ethnicity, education, insurance status, Medicaid status and living arrangement. A dummy variable was used to identify community-dwelling beneficiaries who were permanently institutionalised after the onset of their panel membership.
Beneficiary health attributes
Dummy variables indicating fair to poor health versus good to excellent health were specified from self-reported health information. Self-reported health conditions and Medicare claims data were used to construct a count (0–12) of chronic conditions from a list that included: stroke, cancer, diabetes, rheumatoid arthritis, chronic pulmonary obstructive disease, osteoarthritis, Alzheimer's disease and related dementias, high blood pressure, arteriosclerosis, peripheral vascular disease, ischaemia, and congestive heart failure. Counts of ADLs (0–6) and IADLs (0–6) were included. A third measure, which captured limitations in physical functioning (difficulty with stooping or kneeling, lifting 10 pounds, reaching overhead, writing or handling objects, walking 2–3 blocks), was also specified as a (0–5) count. Self-reported weight and height were used to calculate Body Mass Index, which was then specified as a set of dummy variables.
Analytical approach
Bivariate comparisons in baseline characteristics by AME status were examined using χ2 and Student t tests. Multinomial logistic regressions were used to identify risk factors associated with sustaining an AME injury during panel membership, with death or censoring specified as a single, alternative outcome. Population average models (marginal models) were used to examine the long-term consequences of AME on Medicare expenditures over time. Generalised estimation equation (GEE) was used to test for discontinuities (shifts) in the level of the trajectory and changes in slope during and after AME. Kaplan–Meier survival curves were used to estimate differences in mortality associated with sustaining an AME.
Results
Patterns of AME
Table 1 presents baseline sample characteristics for the entire sample and by AME status. Student t tests were used to identify differences by AME status for each of the study variables. The final sample consisted of 12 541 Medicare beneficiaries (table 1). Nearly one in 5 (19%) or 2408 participants experienced at least one AME during panel participation, with 62% of these events identified from outpatient claims data. At the beginning of panel membership, participants were, on average, 76 years of age, women (59%) and married (54%). However, nearly a third of respondents reported living alone (34%). On average, older adults began panel participation with 3.8 chronic conditions, and had less than one ADL or IADL. Three-quarters of the sample reported their initial health to be good or better. The majority (74%) lived in an urban community. Older adults sustaining at least one AME were found at baseline to be older, more often men, and more often from lower socioeconomic backgrounds in comparison with beneficiaries remaining AME-free during the study period. Medicare beneficiaries sustaining an AME were also found, at baseline, to have a greater number of pre-existing chronic conditions, greater limitations in performing ADLs and IADLs, more apt to report fair to poor health, and more likely to be either underweight or overweight. Study participants contributed 47 (SD=15) person-months on average. Because the majority of participants were observed for the entire 60 months, the duration of observation did not differ appreciably by AME status. However, approximately 28% of beneficiaries with an AME died during panel participation, while only 15% of those without an AME died during the study period. In summary, older adults sustaining an AME were more disabled and frail than those not sustaining an AME.
Baseline sample characteristics (mean or percentage) among older adults by AME status
Illustrative case study
To help ground study results, we provide a brief case study of one AME episode of care. The male patient was aged 72 years at the time of initial panel participation, with a history of diabetes, arthritis and hypertension. At baseline, the patient had difficulty walking and transferring within the home, and was unable to shop or prepare meals unassisted. Prior to the AME, the patient's medical use pattern was modest, and reflected physician visits only. However, during the patient's 33rd month of participation, an incidence of sudden respiratory distress occurred that led to several outpatient visits over a 3-day period, which eventually led to emergency transport for complications involving a cardiac medical device failure. The patient was then admitted for a 7-day inpatient stay from the emergency department. During hospitalisation, a procedure to repair/replace the failed device was observed. Following discharge to home, the patient fell twice, and eventually was hospitalised a second and third time over the next 60 days for issues related to the first hospitalisation (wound not healing), and further complications, including adverse effects of anticoagulant therapy, pneumonia and septicaemia. The third hospitalisation resulted in discharge to an Skilled Nursing Facility (SNF), which ended in death 8 months later.
AME risk factors
Multinomial logistic regressions indicated that several factors increased the risk of sustaining an AME (table 2). Male participants held a 40% greater risk (OR=1.40, 95% CI 1.27 to 1.54) than female participants. With each additional month of age, odds of sustaining an AME increased by 1%, after adjusting for other factors. African-Americans were found at a higher risk (OR=1.19, 95% CI 1.01 to 1.40) than Caucasians. The number of pre-existing chronic conditions, the number of ADL impairments and respondent reports of poor to fair health were all associated with a greater risk of sustaining an AME. Risk of AME increased 27% (OR=1.27, 95% CI 1.24 to 1.29) with each additional chronic condition, after adjusting for other risk factors. In comparison with respondents who reported good to excellent health at the start of their panel membership, those reporting poor to fair health had a 32% greater OR of sustaining an AME. Respondents reporting greater impairment in performing ADLs were also found to have elevated ORs in comparison with other similar Medicare beneficiaries (OR=1.04, 95% CI 1.00 to 1.09). Overall, risk of AME was greater among those in poorer health.
Logistic regression results: risk of AME among older adults associated with beneficiary attributes, health attributes and region of residence (n=428 373 person-months)
Healthcare expenditures associated with AMEs
Table 3 presents estimates from the Base and Fully-Specified GEE Population Averaged Models. Because the Base Model (left-hand columns) only includes dummy variables indicating AME status, results reflect population averages of monthly Medicare expenditures over time. This model suggests that unadjusted Medicare expenditures in the first quarter of panel participation were, on average, $463 dollars (exp(6.14)-1, p<0.0001). The growth rate in quarterly Medicare expenditures exhibited a modest increase over time (b=0.005, p<0.0001), implying an average annual increase of 1.92% (0.48% each quarter). Medicare expenditures during an AME episode increased sharply and remained higher than would have otherwise been expected in quarters following an AME episode. For example, in comparison with pre-AME months, unadjusted Medicare expenditures were, on average, 926% higher during quarters with an AME, and expenditures remained, on average, 353% higher during post-AME quarters. Although expenditures remained significantly elevated in post-AME quarters, the rate of growth attenuated over time, with estimates from the interaction term ((months following AME)*time) suggesting that Medicare expenditures decreased 1.62% (β=−0.016, p<0.0001) on average with each additional month of post-AME history. However, this rate of change was too small to return Medicare growth lines to pre-AME expected trajectories.
Long-term Medicare costs associated with AME
To further explore the effect of injury status on Medicare expenditures over time, a Fully-Specified Population Averaged Model (right-hand side, table 3) used a rich set of covariates to adjust for individual differences in socioeconomic status, health status and physical functioning levels. Although estimates of the fixed- and random-effects were attenuated after casemix-adjustment, suggesting that change in Medicare expenditures over time was explained in part by individual-level differences, a comparison of variance components across models suggests that AME status remains an important determinant of variation in Medicare expenditures among participants. For example, after casemix-adjustments, Medicare expenditures were still observed to increase 744% during AME episodes, while Medicare expenditures remained more than 257% higher in post-AME months than those without an AME. Overall, AMEs increased Medicare spending both in the short-term during the episode of care, as well as in the long run, with the consequences of AMEs among older adults extending well beyond the period typically considered to be an acute episode of care.
Survival analysis
Although it was anticipated that AMEs would be associated with an increased risk of death, the size of the effect was larger than anticipated, particularly given the sizable number of AMEs that originated outside of the acute care setting (62%). Thus analyses were conducted to shed further insight on the relationship between AMEs and risk of death. Kaplan–Meier survival estimates suggest a much steeper attrition rate among beneficiaries with actual AME episodes (figure 2). For example, although nearly 95% of those remaining AME-free survived at 20 months, less than 80% of those sustaining an AME did so. By 50 months, only 60% of the sample sustaining an AME were estimated to have survived, while among beneficiaries free of AMEs, nearly 85% survived. By the end of the period of study participation, only 55% of the sample sustaining an AME survived, whereas nearly 80% of those without an AME were estimated to have survived.
Kaplan–Meier survival estimates following adverse medical event (AME) or randomly assigned (proxy) AME.
Discussion
Findings presented here are among the first to use nationally representative data to explore older adults’ risk of and outcomes following an AME. Our focus on AMEs across medical settings provides insight into the long-term impact of AMEs by using episodes of care that more closely reflect patterns of healthcare service use by older adults with public health implications in terms of ongoing patient safety concerns.34 AMEs are a relatively frequent occurrence among Medicare beneficiaries, with roughly 20% of older adults in this study experiencing at least one AME during the study time period. Risk of AMEs was greater among beneficiaries in poorer health, perhaps capturing, at least in part, the complexity of medical needs associated with managing multiple comorbidities as well as perhaps the frequency with which older adults with chronic care needs access medical services.
These findings are particularly important given public health efforts to improve patient safety,35 reduce costs36 and improve transitions across care settings following implementation of the Affordable Care Act.37 For example, although several studies have sought to investigate AMEs in ambulatory care settings, with at least one study exploring hospital admissions following AMEs arising during ambulatory care,38 much of this effort has been limited to select healthcare providers, settings and/or a single year of study. Unlike most studies to date, we examined the AMEs across medical settings—a definition that is likely to be more applicable to the healthcare service use patterns of older adults. Older adults are frequent users of the healthcare system10 ,39 and often have complex medical needs.40 Because more than half of all AMEs among older adults are identified outside of hospital settings, efforts to reduce preventable AMEs among older adults will require considering both inpatient and outpatient settings as well as the longitudinal nature of healthcare provided to older adults.
Our study has certain limitations. Although our approach using latent class analysis demonstrated strong test–retest reliability to measure AME severity, we did not distinguish between likely preventable and non-preventable events over episodes of care, and with respect to specific locations of care (eg, physician settings, emergency department settings, outpatient surgery). Our results may not fully distinguish outcomes associated with the medical care required at the time of AME from the actual effects of the AME. However, the use of population average models provides some ability to disentangle the two. The conventional strategy of allowing naturally defined episodes based on the continuous observation of ICD-9 codes in medical claims was insufficient for AME identification, in part, because the medical care responsible for the AME could end on one claim (eg, a hospital claim), but the AME may not be visible until the respondent accessed the healthcare system again, often in another setting (eg, physician's office). Although we responded to this difficulty by using a conventional approach to constructing episodes (eg, adding 1-month prior and 1-month post AME to create 3-month episodes), it is likely that additional effort to refine episode definition across medical settings is necessary to better describe and capture the effect of AMEs on older adult outcomes over time.
Conclusions
Overall, study findings indicate that AMEs pose significant risk to the health and well-being of older Medicare beneficiaries, while the effects of AMEs are observed long after the initial episode has concluded. Despite including less medically severe cases (eg, ambulatory-care AMEs), the effects of AMEs on beneficiaries’ Medicare expenditures and survival risk in the long run are both severe and long-term in nature, perhaps reflecting the complexity of medical needs managed over multiple healthcare settings. Because more than half of AMEs were identified outside of hospital settings, efforts to reduce preventable AMEs among older adults and improve patient safety require public health efforts that target both inpatient and outpatient healthcare settings.
What is already known on the subject
-
Older adults are vulnerable to adverse medical events (AMEs) with poor outcomes following AMEs.
-
A paucity of information exists about the occurrence of AMEs among older adults across the healthcare continuum as well as the long-term impact of AMEs on older adult outcomes.
What this study adds
-
Nearly 19% Medicare Current Beneficiary Survey participants experienced at least one adverse medical event (AME), with 62% of these events identified from outpatient claims.
-
The impacts of AMEs are observed over extended periods of time and are associated with considerable excess mortality and costs, long after the initial episode concludes.
Texas construction workers more likely to be killed on the job
An analysis of workplace data from 2003 through 2012 found that Texas has exceptionally high rates of fatal injuries in specialty construction trades. Texas's 4593 occupational deaths over the decade is 579 more than would have been expected based on US averages. In comparison, California had 1204 fewer deaths than expected. Researchers claim government and industry in Texas have invested relatively little in safety equipment, training and inspections. The Dallas Morning News (noted by IBP).
Multimillion dollar prevention scheme failing in New Zealand
The New Zealand Accident Compensation Corporation is doubling funding for failing injury prevention schemes. Still there are concerns that the changes may neglect some dangerous industries. The prevention budget for agriculture, construction, forestry and manufacturing has nearly been cut in half. In contrast, road safety has been increased substantially. (noted by IBP).
Bike share and helmet issues
Some statistics suggest that bike share programmes are remarkably safe, perhaps because the bikes are sturdy, slow and reliable. King County, Washington has had a mandatory helmet law since 2003 and is initiating a bike share programme. Helmet-dispensing kiosks will appear at all bike-share station. Helmets can be rented for $2 for 24 h and will be sanitised after every use. (noted by IBP).
Acknowledgments
A preliminary draft of this paper was presented at the 64th Annual Scientific Meeting of the Gerontological Society of America.
References
Supplementary materials
Press release
Files in this Data Supplement:
Footnotes
-
Contributors Substantial contributions to the conception or design of this work and data acquisition were made by MWC and FWP. Substantial contributions to data analysis and interpretation were made by all authors. MWC led the analysis. MWC and MZ led the drafting of the article and all authors were involved in revising it and approving the final version to be published.
-
Funding This work was supported by National Institutes of Health/National Institute on Aging, NIH/NIA Contract R21AG031983.
-
Competing interests None.
-
Provenance and peer review Not commissioned; externally peer reviewed.
-
Data sharing statement Data for this work were drawn from the Medicare Current Beneficiary Survey (MCBS). Parties interested in obtaining MCBS data are referred to the Research Data Assistance Center (ResDAC).